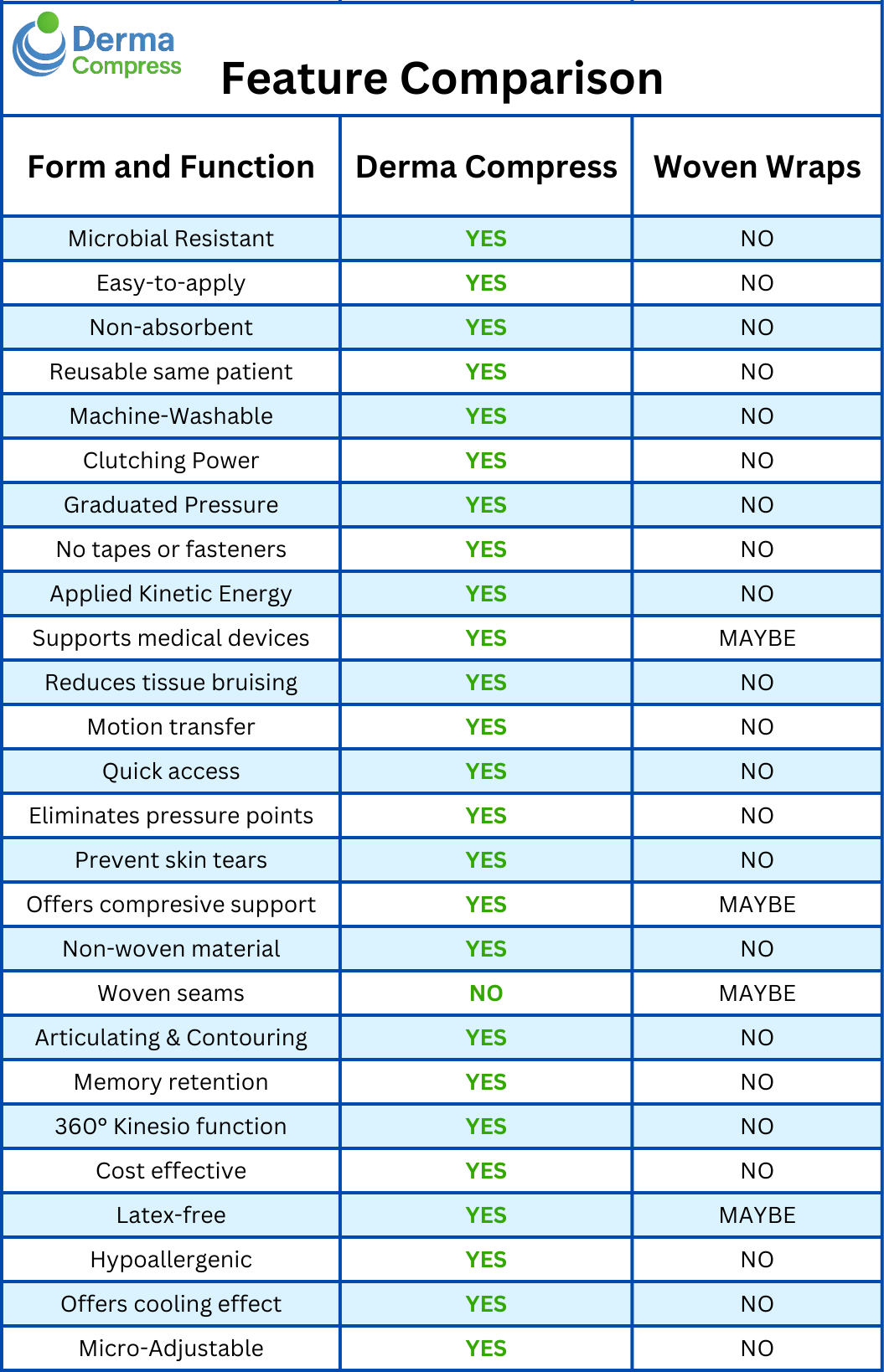
NOVEL COMPARISON OF A MICROBIAL-RESISTANT COMPRESSION AND SECUREMENT DEVICE VERSUS TRADITIONAL GAUZE WRAP SHOWING POSITIVE IMPACT ON WOUND HEALING IN POOR AND DISADVANTAGED PATIENTS
JOSEPH G. SMITH DPM, ALL AMERICAN PODIATRY & WOUND CARE, VIRGINIA BEACH, VA
Abstract
Lack of access to adequate wound care supplies can have a detrimental effect on the general patient population's ability to heal a wound which many times progresses to infection, especially among poor and disadvantaged patients. In the US annually 8.2 million Medicare beneficiaries have a chronic non-healing wound at a cost of over 531 billion dollars annually. More than 7 million elderly people live below the poverty level (1). Many times lack of adequate bandaging supplies will lead to failure of typica topical wound care treatments as well and represent the nidus for infection and a pathway of potential progression to life threatening infection.
Introduction
Based on the 33 pounds of waste produced from each staffed bed every day, U.S: hospitals produce more than 5.9 million tons of medical waste each year. And that doesn't include medical waste from medical, dental, veterinary, pharmacy, home care and other small quantity generators across the country(2).

This bandage system is ideal for managing:
Pressure and venous stasis ulcers
Diabetic wounds
Arterial insufficiency ulcers
Neuropathic ulcers
Traumatic wounds
Surgical wounds
Skin tears
1st and 2nd degree burns
Skin grafts (donor and recipient sites)
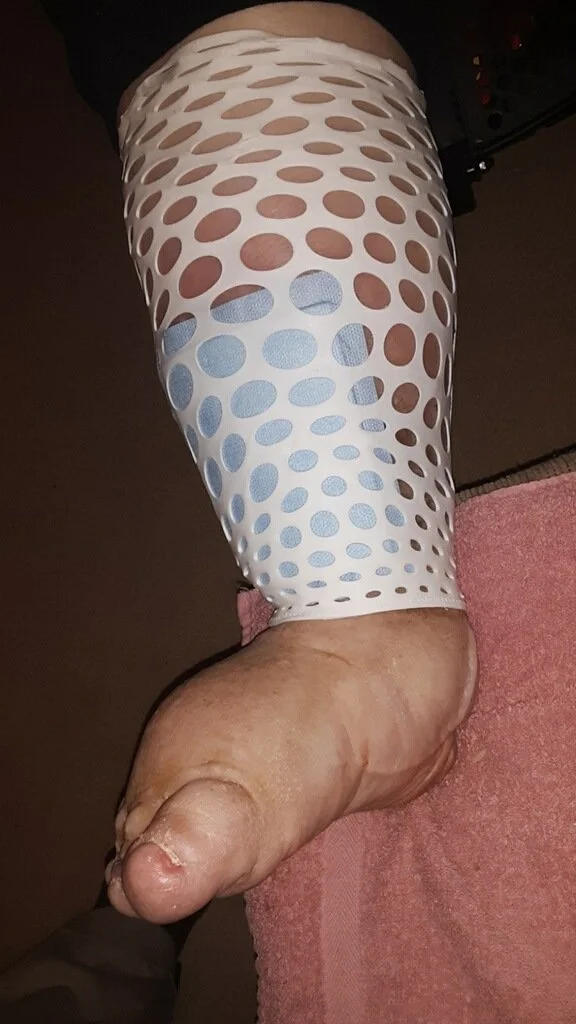
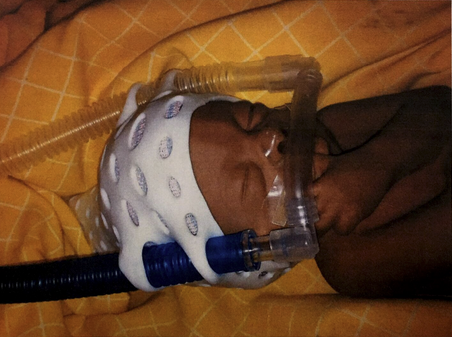
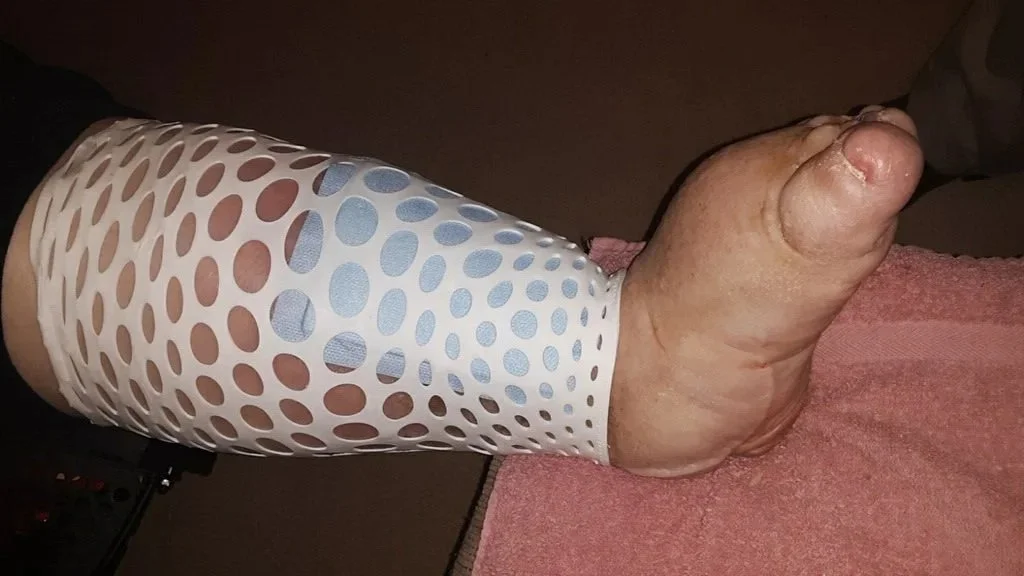
Patient benefits include:
Prevention of skin tears
Reduces bruising of thin and fragile tissue
Easy access for wound and burn treatment and inspection
Promotes airfiow (vented product)
Soft and gentle feel with a "cooling" effect
Consistent and even pressure over wounds
Available in short and long: solid and vented; low, medium and high compression strengths
Methods and Materials
For this work, traditional bandage systems will be compared to a microbial-resistant compression and securement device evaluating for cost differences as well as time of application. Traditional bandage systems will be compared to one which is designed to be reusable on the same person and supports solt tissue, muscles, and joints and aids in mobility and recovery. This modern approach will be shown to protect, support and assist in wound healing in a hypoallergenic fashion versus traditional cotton gauze wraps. We will also compare the length of time for dressing changes using the modern versus traditional methods. For this research we used kling and kerlix versus the modern bandage which is easy-to-apply, non-absorbent, hand washable and reusable on the same patient. This non-woven tubular compression device is also microbial-resistant to Staphylococcus aureus and Pseudomonas aeruginosa, It holds dressings and medical devices in place without the use of sticky tapes, messy adhesives and clumsy fasteners. The modern system is wound and burn protective, water and fluid resistant, non-woven, and latex-free.
Conclusions
Three groups of health care providers were used in a randomized double-blind, muiti-center trial. The groups were broken up as follows: expert, mid-level, and novice with regards to expertise in wound care and bandage application. The clinicians were timed applying both the modern bandage system and the traditional method. In all three instances the modern system cut the bandage application time by greater than 50% across the board.
As this bandage is reusable indefinitely, the initial cost is the only cost versus the cost of daily bandage systems. This not only decreases the amount of biohazardous waste, but markedly decreases the fiduciary responsibility of the health care system as a whole.
Results
Treating patients using a microbial-resistant compression and securement device can have a positive impact on wound healing and infection modulation in poor and disadvantaged patients and can restore patients to a healing state and decrease the potential progression to infection when compared to traditional bandage systems due in part to their ability to be reused. The amount of time to do a standard dressing change has also been shown to decrease markedly while using the modern bandage system. This system also uses no daily disposable material, which leads to less biohazardous waste.